How Long Does It Take To Go Blind From Cataracts

My Grandma Elsie, bless her heart, always had a twinkle in her eye. And for a good few years, that twinkle was accompanied by a rather dramatic squint. She’d hold her knitting so close to her nose it was practically a facial massage, and reading the newspaper required a magnifying glass the size of a frisbee. “Oh, it’s just my eyes getting old, dearie,” she’d say with a dismissive wave, as if it were as mundane as a creaky knee.
But it wasn’t just her eyes getting old. It was a slow, insidious creeping of something else, something that eventually made that twinkle a lot harder to see. And that, my friends, is what we’re going to chat about today: cataracts. Specifically, the age-old question that I’m sure has crossed your mind, perhaps while squinting at a blurry street sign yourself: How long does it actually take to go blind from cataracts?
Let’s be honest, the phrase “go blind from cataracts” sounds pretty darn final, doesn't it? It conjures images of utter darkness, like a light switch being flipped off permanently. And for some, that might be the ultimate trajectory if left unchecked. But here's the thing, and it's a crucial distinction: cataracts are rarely an overnight sensation. They’re more of a slow-burn, a gradual dimming of your world, like a vintage film projector starting to sputter.
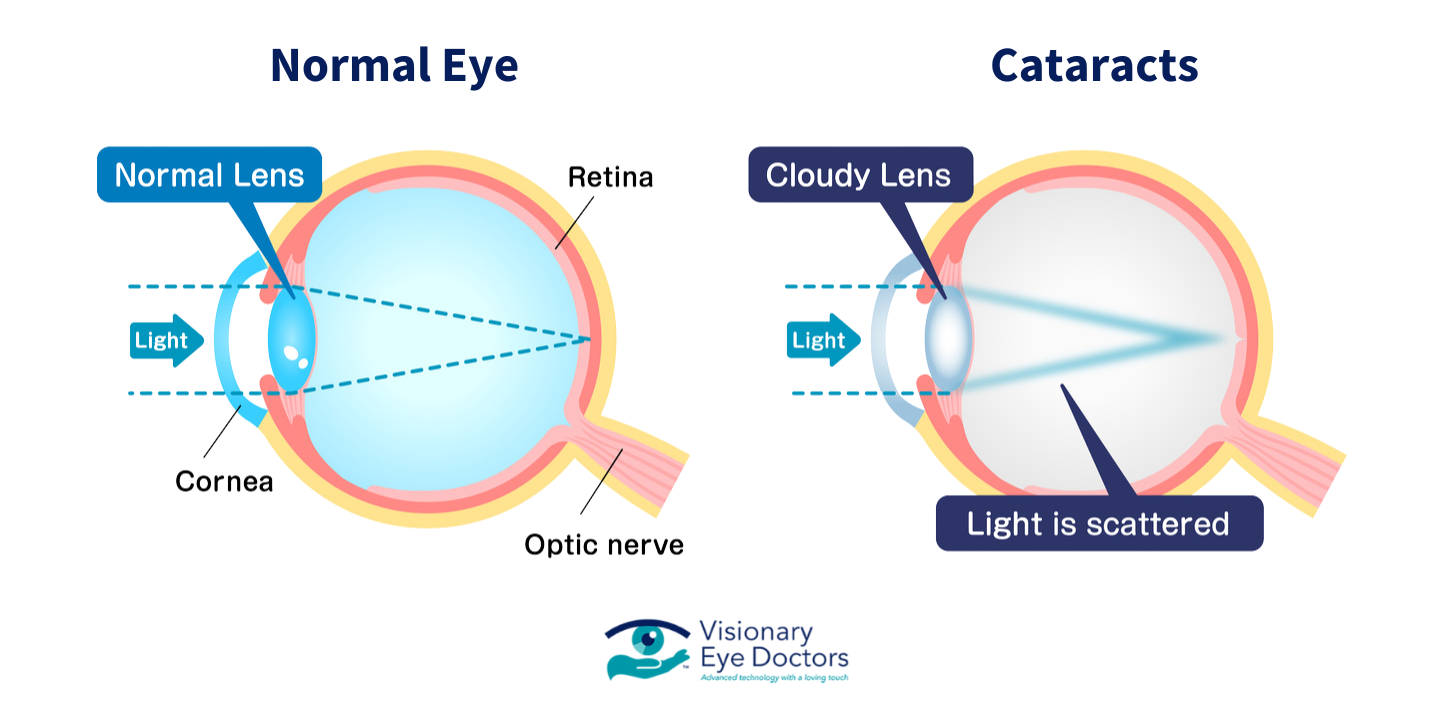
Think of your eye’s lens like a perfectly clear, perfectly flexible magnifying glass. It’s designed to focus light onto your retina, giving you crisp, clear vision. Now, imagine that magnifying glass slowly clouding over. Not all at once, mind you. It’s more like a fine mist settling in, then gradually thickening. That’s your cataract forming. And that cloudiness? That’s what’s interfering with the light getting to where it needs to go.
So, to directly answer the burning question: There's no single, definitive timeline for going blind from cataracts. It’s not like a ticking clock that sounds the alarm after, say, five years. It's a highly individualized process, influenced by a whole bunch of factors. Some people might notice changes relatively quickly, maybe over a few years, while others can live with them for decades without significant vision loss.
What are these mysterious factors, you ask? Well, it’s a cocktail of things, really. The speed at which a cataract progresses is influenced by:
1. The Type of Cataract
Did you know there are different kinds of cataracts? Yep, it's not just one generic cloud. The most common type, nuclear cataracts, tend to develop very slowly in the center of the lens. Think of it like the lens getting a bit yellow and harder over time. This can cause a gradual increase in nearsightedness (or a worsening of existing nearsightedness) and some blurriness. It’s often the one that Grandma Elsie was dealing with, that slow dimming.
Then there are cortical cataracts, which start as wedge-shaped opacities on the outer edge of the lens, spreading inwards. These can cause glare and halos around lights, which can be particularly annoying when driving at night. Imagine little starbursts emanating from every headlight – not ideal!
Posterior subcapsular cataracts, on the other hand, are a bit more of a speedy Gonzales. They form on the back surface of the lens and can progress quite rapidly, especially in people with diabetes or those who have taken certain medications like corticosteroids. These can cause significant visual impairment in a shorter period. So, if you have underlying health conditions, it’s definitely something to keep an eye on (pun intended, of course).
2. Genetics and Family History
Ah, genetics. The great influencer of pretty much everything, isn't it? If cataracts run in your family, you might be more predisposed to developing them, and sometimes, they can progress a little faster. It’s like being dealt a certain hand of cards, and your eyes are part of that game.
3. Lifestyle Factors
This is where you have a bit more control, which is always good news! Things like:
- Exposure to UV light: Just like you need sunscreen for your skin, your eyes need protection too. Prolonged, unprotected exposure to the sun’s UV rays is a major risk factor. So, wear those sunglasses, people!
- Smoking: Yeah, sorry to be the bearer of bad news, but smoking is linked to a higher risk and faster progression of cataracts. It’s just one more reason to kick the habit.
- Diabetes: As mentioned earlier, diabetes is a big one. High blood sugar levels can affect the lens, leading to faster cataract formation. Managing your diabetes is key here.
- Certain medications: Long-term use of corticosteroids can accelerate cataract development. If you’re on these, definitely have a chat with your doctor about eye health.
So, while there's no universal "going blind" date, we can talk about the stages of cataract development and how they affect vision.
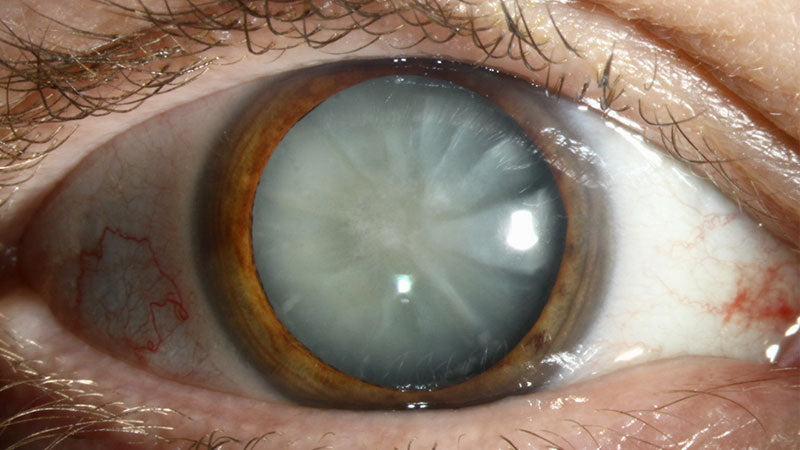
The Gradual Dimming: Stages of Cataract Vision
Let’s break it down, because understanding the progression can demystify the whole process.
Stage 1: The Subtle Shift
In the early stages, you might not notice much at all. Or, if you do, it's so minor you’ll probably dismiss it. Perhaps colors seem a little less vibrant, or you start needing a bit more light to read. You might find yourself squinting more, just like Elsie. It’s the kind of thing you might blame on being tired or just a natural part of aging. Your optometrist might even see it during a routine check-up before you’re fully aware of it.
This is usually when the lens starts to develop a slight yellow tint or a few small opacities. It’s like a tiny smudge on your glasses that you can almost ignore.
Stage 2: The Noticeable Nuisance
This is where things start to become a bit more inconvenient. You might notice:

- Blurry or hazy vision: Text on signs, books, or computer screens might become difficult to read.
- Increased sensitivity to glare: Headlights from oncoming cars can seem blinding, and sunlight can be overwhelming. Halos might appear around lights.
- Difficulty seeing at night: Driving after dark can become genuinely challenging.
- Colors appearing faded or yellowish: White fabrics might look dingy, and vibrant colors might seem muted.
- Frequent changes in eyeglass prescription: Your optometrist might be adjusting your prescription more often as your vision continues to change.
At this stage, the cataract has grown larger and is significantly impacting how light enters your eye. It’s like trying to look through frosted glass – you can still see shapes and some details, but it’s nowhere near clear.
Stage 3: The Significant Impairment
This is when vision loss becomes a major impediment to daily life. Activities that were once easy, like reading, driving, cooking, or even recognizing faces, become difficult or impossible without significant assistance. Your world can start to feel quite dim and fuzzy.
At this point, the cataract is likely quite dense, significantly blocking light. It can feel like you're constantly looking through a very dirty window. This is when most people seek medical intervention because their quality of life is genuinely affected. It's not about "going blind" in the absolute sense, but about a profound loss of useful vision.
Stage 4: Severe Vision Loss (Approaching "Blindness")
If left untreated for a very, very long time, cataracts can progress to the point where they cause severe vision loss. In extreme cases, the lens can become so opaque that only light perception remains. This is the scenario that most people fear when they hear "blindness from cataracts." However, it’s important to reiterate that this is rare in developed countries due to the availability of regular eye exams and effective treatment.
Think of it as the magnifying glass being completely opaque, like a solid block of milky glass. Light might get through, but no images can be formed. Fortunately, with modern medicine, this stage is largely avoidable.

When is it "Time"? The Decision to Treat
So, how long does it take to reach these later stages? As we’ve established, it’s a spectrum. For some, the subtle shifts might start in their 40s or 50s, and by their 70s or 80s, they might be in Stage 2 or 3. For others, it might be a much slower journey, and they might reach a very advanced stage only in their late 80s or 90s, if at all.
The crucial point is that cataracts are treatable. And the decision to treat isn't necessarily dictated by how long it's been developing, but by how much it's affecting your life. Your ophthalmologist won’t just say, "Oh, you've had that for 10 years, it's time to operate." Instead, they'll ask about your symptoms and how they impact your daily activities. If you're struggling to read, drive safely, or recognize people, it’s likely time to discuss treatment options.
The surgery itself is remarkably safe and effective. Essentially, the clouded lens is removed and replaced with a clear, artificial intraocular lens (IOL). It’s a relatively quick procedure, and the recovery is usually quite smooth. People often report their vision being significantly clearer almost immediately after the surgery. Imagine going from looking through a smudged window to having a brand-new, crystal-clear pane of glass – that’s the kind of difference it can make.
Grandma Elsie eventually had her cataracts removed in her late 80s. The twinkle in her eye? It came back with a vengeance, brighter than ever. She could read her books without the giant magnifying glass, and knitting became a joy again, not a strenuous visual workout. She often joked that she could suddenly see all the dust bunnies she’d been missing for years!
So, the next time you find yourself squinting, or wondering about that gradual dimming, remember that cataracts are a common part of life for many. They don't typically lead to sudden blindness, but rather a slow, progressive decline in vision. The "how long" is a very personal journey, but the good news is that with regular eye check-ups and timely intervention, you can ensure that twinkle in your eye, and the clarity of your world, lasts for a very, very long time. Don't wait until you can't see the dust bunnies, folks! Get those eyes checked!
