How Long Does It Take To Heal A Broken Metatarsal
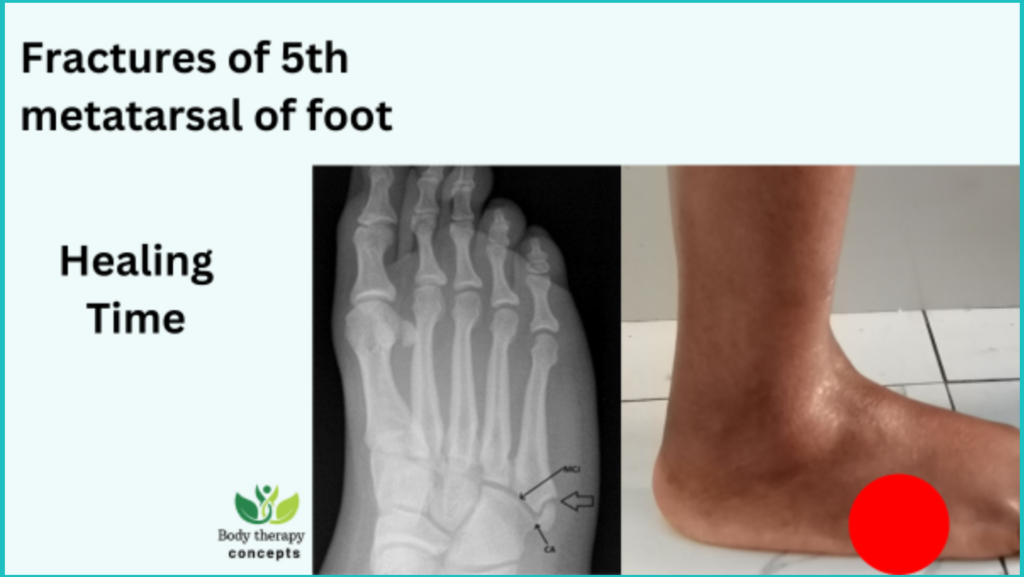
So, you’ve managed to join the not-so-exclusive club of metatarsal mishaps? Welcome! It’s a common rite of passage, really. Whether it was a clumsy encounter with a rogue piece of furniture, a daring (or perhaps not-so-daring) sports move gone awry, or just a particularly enthusiastic dance session that ended with a little too much floor impact, a broken metatarsal can really put a damper on your rhythm. But before you start imagining months of hobbling around like a hobbit on a quest, let's dive into the nitty-gritty of how long this whole healing gig actually takes. Think of this as your chill guide to getting back on your feet, sans the drama.
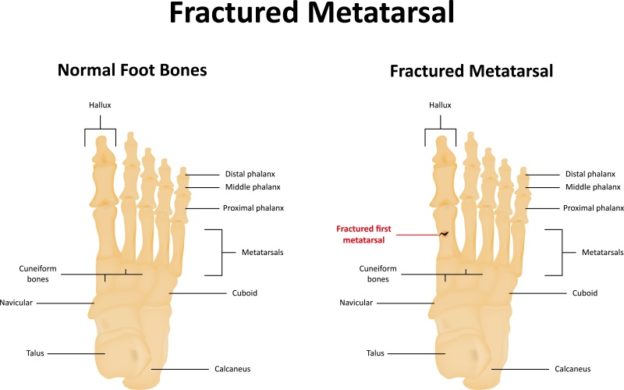
First things first, let’s get acquainted with our unsung heroes: the metatarsals. These are the five long bones in the middle of your foot, running from your ankle to your toes. They’re the workhorses that help you walk, run, jump, and generally navigate the world. When one of these guys decides to take a break – a literal break – it’s their way of saying, "Hey, I need a minute!" And that minute, or rather, that collection of minutes that adds up to weeks and months, is what we’re here to talk about.
The million-dollar question, of course, is: how long does it take to heal a broken metatarsal? The short answer? It’s a bit of a spectrum, my friend. Most uncomplicated fractures, the kind that aren’t displaced (meaning the bone pieces are still nicely aligned), tend to heal within 6 to 8 weeks. Think of this as the average pace, the standard speed on the healing highway.
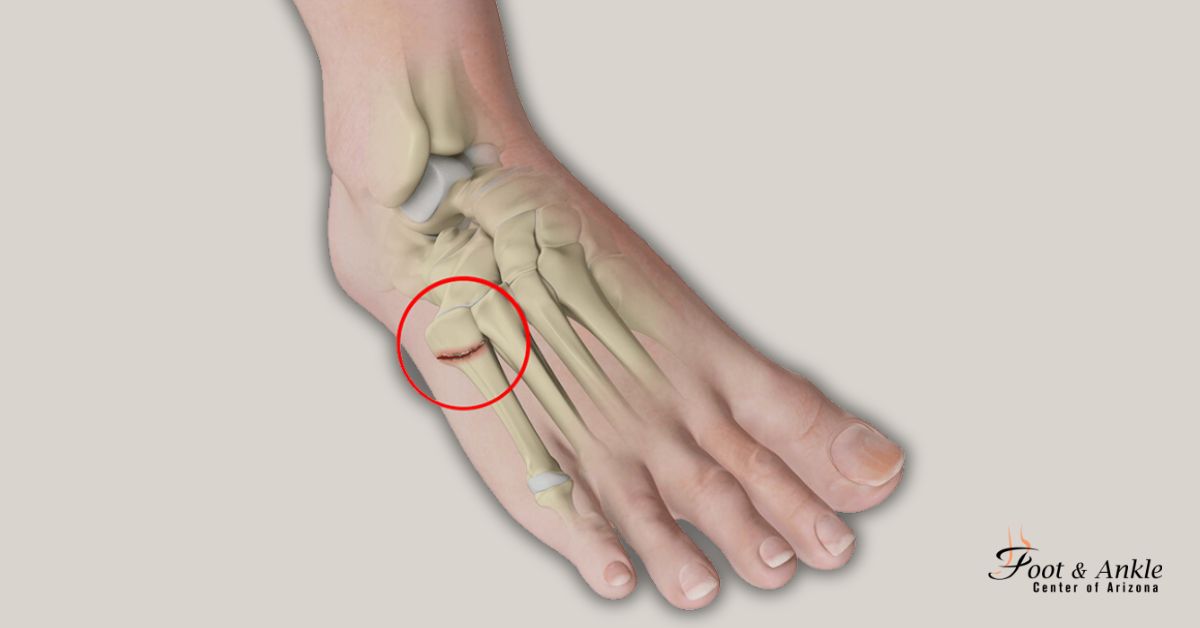
But, and there’s always a but, right? This timeframe can be influenced by a bunch of factors. It's not a one-size-fits-all situation. For instance, the location of the fracture matters. Some metatarsals are tougher than others, and fractures in certain spots might take a tad longer to mend. The severity of the break is another biggie. A hairline crack is going to behave differently than a bone that’s completely snapped in two.
Then there’s your own body chemistry. You know, that secret sauce that makes you you. Things like your age, overall health, and even your nutrition can play a role. A younger, healthier individual with a diet rich in calcium and Vitamin D might find their bones knitting back together a bit more efficiently than someone with pre-existing conditions or a less-than-ideal diet. It’s like your body is its own little construction crew, and some crews are just naturally faster builders.
The Phases of Foot Recovery: A Gentle Timeline
Let’s break down the healing journey into a few digestible stages, shall we? This isn't a race, but understanding the phases can make the whole process feel less like a mystery and more like a guided tour.
Phase 1: The Initial "Ouch!" and Rest (Weeks 1-3)
This is the immediate aftermath. Expect some pain, swelling, and that distinct feeling of “uh oh.” Your doctor will likely recommend rest, ice, compression, and elevation (RICE) – the classic quartet of injury management. You might be sporting a snazzy boot or crutches. Embrace the drama! Think of it as your temporary superhero stance. This phase is all about protecting the injured bone and allowing the initial inflammatory response to do its thing. Your body is already starting to lay down the groundwork for repair.
Phase 2: The "Can I Move Yet?" Stage (Weeks 3-6)
If things are progressing well, your doctor might start encouraging some gentle movement. This could involve gradual weight-bearing as tolerated, or physiotherapy. The goal here is to avoid stiffness and maintain as much mobility as possible without re-injuring yourself. Think of it as coaxing the construction crew to start putting up the scaffolding. It’s still delicate work, but progress is happening.

Phase 3: Getting Back in the Game (Weeks 6-8 and beyond)
This is where things really start to pick up. You’ll likely be transitioning out of your boot and onto your own two feet, perhaps with the aid of supportive shoes or orthotics. Physiotherapy will become more focused on strengthening, balance, and regaining full function. This is the phase where you start to feel like yourself again, albeit a slightly more cautious version. It’s the crew finishing up the interior design and making the place livable again.
What Can Slow Down the Healing Process?
Now, while we’re aiming for that sweet 6-8 week mark, it’s important to be aware of potential speed bumps. Sometimes, healing can take a bit longer, and it’s not always anyone’s fault. For instance, if your fracture was more serious – say, a displaced fracture where the bone ends aren’t aligned, or a comminuted fracture where the bone is in multiple pieces – it will naturally take more time and potentially medical intervention like surgery to set things right.
Then there are those lifestyle factors we touched on. Smoking, for example, is a notorious enemy of bone healing. Nicotine constricts blood vessels, which can reduce the blood supply to the healing bone, hindering the process. So, if you’re a smoker, this might be the universe’s not-so-subtle nudge to consider quitting. Your bones will thank you.
Certain medications can also play a role. Steroids, for instance, can sometimes impede bone repair. If you’re on long-term medication, it’s always worth a chat with your doctor about how it might affect your recovery.
And let’s not forget about infection. While rare, if your fracture was an open fracture (where the skin was broken) or if there are any signs of infection, this can significantly delay healing and require aggressive treatment. Your body is a complex ecosystem, and keeping it clean and healthy is paramount.
The Role of Your Doctor and Physiotherapist: Your Healing Dream Team
You’re not in this alone! Your medical team is your A-team for recovery. Your doctor will diagnose the fracture, determine its severity, and recommend the appropriate treatment plan, whether that’s casting, bracing, or surgery. They’ll be your guide through the initial stages and monitor your progress.
Then there’s your physiotherapist. These folks are pure magic. They’ll work with you to regain strength, flexibility, and balance. They’ll design personalized exercises to help you get back to doing the things you love, whether that’s hiking, dancing, or simply walking the dog without a wince. Don't underestimate the power of a good PT session; it's where the real transformation happens.
Cultural Tidbits: When Feet Went on Strike
Interestingly, the concept of immobilizing a broken limb isn't exactly new. Ancient Egyptians were pretty clued into basic bone setting techniques. They’d use splints made from linen and wood to keep fractures stable. So, while we’ve got our fancy boots and advanced imaging, the fundamental principle of giving a broken bone time and support remains the same across millennia. It’s a testament to our bodies’ innate ability to heal.
Think about it: throughout history, people with broken legs or feet had to rely on their communities for support, literally. They couldn’t just hop to the store for groceries. This probably fostered a deeper sense of interdependence and perhaps a greater appreciation for mobility when it returned. We’re still figuring out the best ways to navigate this, but our modern approach is definitely more comfortable than a bunch of reeds and linen!
Practical Tips for a Smoother Recovery
Alright, let’s get down to the nitty-gritty of making this recovery period as smooth as possible. Because let's be honest, a broken metatarsal can feel like a major inconvenience, but with a few smart strategies, you can navigate it with more grace than you might think.
Listen to Your Body: This is paramount. If something hurts, don’t push it. Your body is sending you signals, and ignoring them is like trying to drive a car with the “check engine” light on. Gradually increase your activity levels as advised by your doctor and physiotherapist. It’s about progress, not perfection.
Nutrition Matters: As we mentioned, your diet is your bone’s best friend. Load up on calcium-rich foods like dairy products, leafy greens (kale, spinach), and fortified foods. Don’t forget Vitamin D, which helps your body absorb calcium. Sunshine is a great source, but you can also find it in fatty fish like salmon and fortified milk. Think of it as fueling your body’s construction crew with the best building materials.
Stay Hydrated: Seems simple, right? But staying well-hydrated is crucial for overall bodily function, including circulation and cell repair. Keep that water bottle handy!
Manage Pain Wisely: Your doctor will likely prescribe pain relief. Use it as directed. Beyond medication, consider techniques like meditation or mindfulness to help manage discomfort and reduce anxiety about the healing process. Sometimes, a good playlist and a comfortable spot on the couch are all you need for some therapeutic chill.
Get Moving (Smartly): Once cleared by your healthcare provider, embrace gentle exercises. This could be anything from simple ankle pumps and toe curls while sitting to progressive weight-bearing. Even small movements stimulate blood flow, which is essential for healing. If you're cleared for it, consider pool therapy – the buoyancy of water can be a game-changer for gentle movement.
Invest in Good Footwear: Once you’re out of the boot, supportive shoes are your best friend. Look for shoes with good arch support and cushioning. Your physiotherapist can offer recommendations, and sometimes custom orthotics can provide that extra bit of support your foot needs as it regains its strength.

Patience, Grasshopper: This is perhaps the hardest tip to follow, but the most important. Healing takes time. There will be days when you feel great and days when you feel like you’re back at square one. That’s normal. Celebrate the small victories – being able to walk a little further, feeling less pain, or successfully completing a physio exercise. These are all signs of progress.
When to Seek Further Advice
While most metatarsal fractures heal without major complications, it’s always wise to know when to ring your doctor. If you experience:
- Increased or severe pain that isn’t managed by medication.
- Worsening swelling or redness.
- Numbness or tingling in your foot or toes.
- Signs of infection, such as fever, chills, or pus.
- Any concerns about your healing progress.
Don’t hesitate to reach out. It’s always better to be safe than sorry, and your medical team is there to support you through any bumps in the road.
Fun Fact: The longest bone in the human body is the femur (thigh bone), but the smallest bone is actually in your ear – the stapes. Your metatarsals are somewhere in the middle, sturdy but definitely not the longest or the shortest!
So, how long does it take to heal a broken metatarsal? The honest answer is that it’s a journey, not a destination with a fixed arrival time. For most, expect a good 6 to 8 weeks of dedicated care and patience. But remember, this is an average, and your unique body will have its own rhythm of recovery.
Ultimately, a broken metatarsal is a temporary detour, not a permanent roadblock. It’s a chance to slow down, reassess, and perhaps even discover a new appreciation for the incredible capabilities of your own body. As you navigate this period, remember to be kind to yourself, trust your healing process, and lean on your support system. Soon enough, you’ll be back to dancing, running, and conquering your world, one step at a time.
