Long Term Effects Of Spinal Compression Fracture
Okay, so imagine this: my Aunt Carol, bless her adventurous heart, decided to take up trampolining at the sprightly age of 75. She swore it was the secret to staying young. Naturally, her family, including yours truly, looked at her like she’d sprouted a second head. “Aunt Carol,” I remember saying, trying to keep a straight face, “are you sure about this?” She just winked and bounced. A few weeks later, she was in the hospital, a grim look on her face, clutching her back. Turns out, her “secret to staying young” involved a rather unplanned and painful landing that resulted in a spinal compression fracture. Not quite the youthful bounce she was aiming for, eh?
It got me thinking, though. We often hear about these fractures, especially with older folks, and the immediate pain is the big, scary thing. But what happens after the initial drama subsides? Is it just a case of “ouch, my back” and then life goes back to normal? Spoiler alert: it’s usually a bit more complicated than that. My aunt’s story, while a bit extreme with the trampolining, is a perfect jumping-off point (pun intended, sorry!) to explore the long-term effects of a spinal compression fracture. Because, let me tell you, it’s not always just about a temporary ache.
So, let’s dive into this, shall we? Think of this as a friendly chat, not a dry medical textbook. I’m not a doctor, so don’t come to me with your prescription refills, but I can certainly help demystify some of the stuff that can linger long after the fracture is healed. Because knowledge, as they say, is power. And understanding what might happen can help you or someone you know navigate this whole process a bit better. And hey, maybe it’ll even help you convince your own daredevil aunt to stick to shuffleboard.
The Immediate Aftermath: More Than Just a Bump
When a spinal compression fracture happens, it’s basically a vertebra (one of those little bones in your spine) collapsing. Ouch. The most obvious symptom, as you can probably guess, is sudden, often intense back pain. This pain can be sharp, stabbing, and it usually gets worse when you move, stand, or walk. Lying down might offer some relief, but even then, it can be a struggle.
But it’s not just about the pain. You might also experience:
- A feeling of tenderness in the affected area.
- A change in posture, like starting to hunch forward.
- Sometimes, a reduced ability to move around freely.
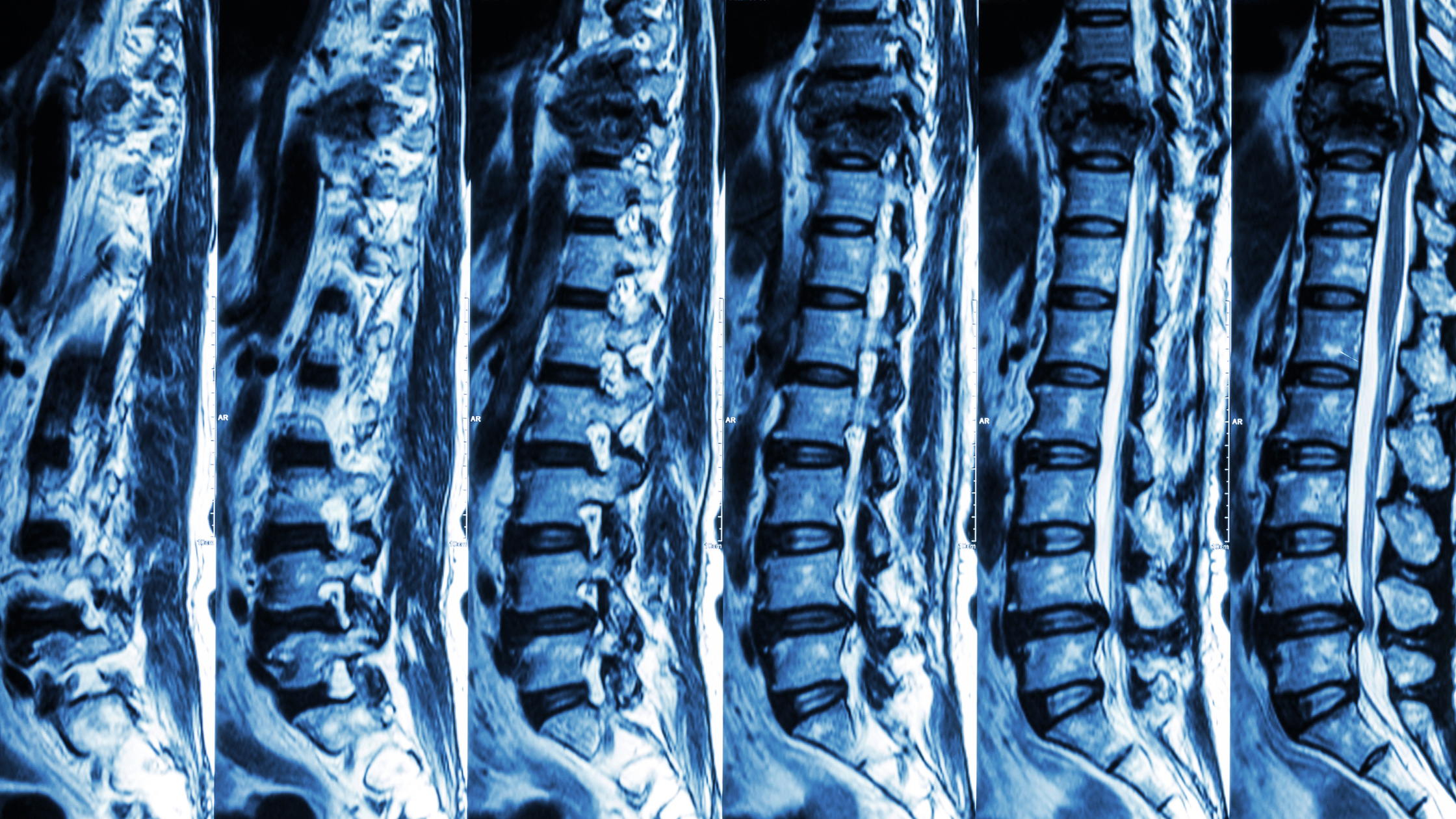
This initial phase is crucial, and it’s where medical professionals come in. Diagnosis usually involves X-rays, CT scans, or MRIs to see exactly what’s going on. Treatment can range from rest and pain medication to more involved procedures depending on the severity. But while everyone is focused on getting you comfortable and fixing the immediate damage, the long game is already in play. The decisions made and the care received during this time can significantly influence what happens down the line. So, yeah, even when you’re just trying to survive the initial pain, you’re already setting the stage for your future back health. Kind of wild, right?
The Ghost of Pain Past: Chronic Pain and Its Buddies
Now, let’s talk about what happens when that acute, “oh-my-goodness-what-was-that” pain starts to fade, but a different kind of discomfort decides to move in permanently. This is where the long-term effects really start to show their faces. One of the most common lingering issues is chronic pain.
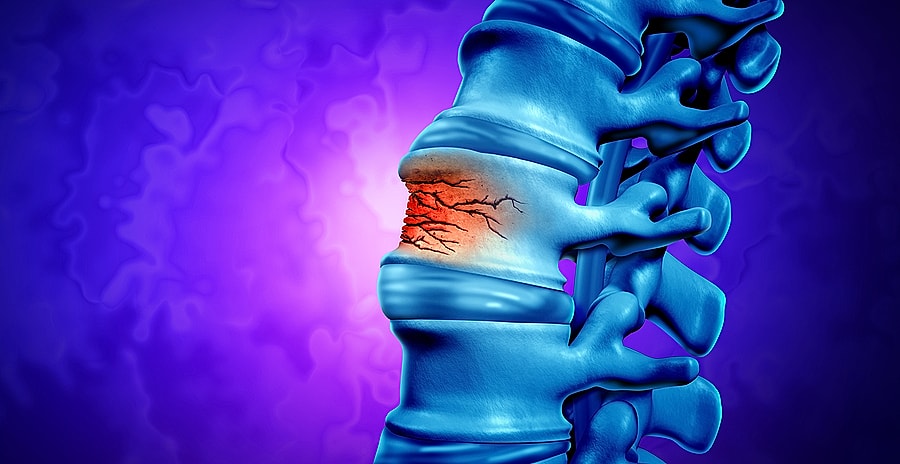
This isn’t your everyday ache. Chronic pain can be dull, throbbing, burning, or even shooting. It can be constant or come and go, but it’s there, making everyday tasks feel like climbing Mount Everest. It can impact your mood, your sleep, your ability to work, and your social life. Imagine not being able to enjoy a simple walk in the park without that nagging pain following you. It’s a real bummer, and it’s a lot more common than you might think after a spinal fracture.
And chronic pain often brings along some unwelcome friends. You might find yourself dealing with:
- Muscle spasms and stiffness: Your body might be trying to protect the injured area by tensing up, which can lead to more pain and restricted movement.
- Fatigue: Dealing with pain 24/7 is absolutely exhausting, both physically and mentally.
- Sleep disturbances: Trying to find a comfortable position to sleep when your back is hurting is a Herculean task. Poor sleep then exacerbates everything else.
It’s like a domino effect, where one problem leads to another, and then another. And if you’re not actively managing these issues, they can really take over your life. My aunt, for example, found that even after her fracture healed, she was constantly tired and her sleep was terrible. She’d wake up stiff and sore, and it would take her ages to get going in the morning. It was a far cry from the energetic woman who loved her trampolining sessions.
The Stoop: Postural Changes and Their Ripple Effects
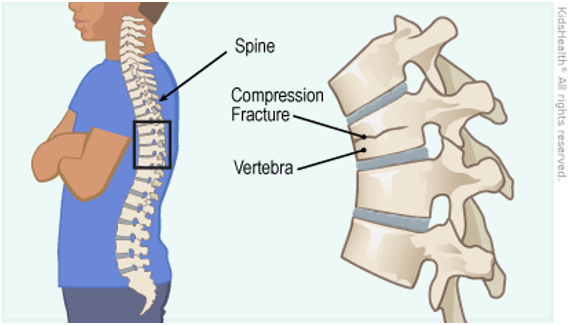
Remember how I mentioned my aunt started looking a bit more hunched? That’s another significant long-term effect. When a vertebra collapses, it loses height. If multiple vertebrae are affected, or if the collapse is substantial, it can lead to a progressive curvature of the spine, often called a kyphosis. You might know it as a dowager’s hump, though it’s not exclusive to women or just the elderly, and it’s certainly not something to be “humped” about – it’s a serious physical change.
This postural change isn’t just about how you look. It can have a cascade of other problems:
- Reduced lung capacity: The compressed chest cavity can make it harder for your lungs to expand fully, leading to shortness of breath, especially with activity. Imagine trying to go for a brisk walk and feeling like you can’t get enough air. Not fun.
- Digestive issues: The altered posture can put pressure on your abdominal organs, potentially leading to problems like heartburn, constipation, or a feeling of fullness.
- Increased risk of further fractures: This is a big one. As your posture changes and your spine becomes less stable, you become more vulnerable to future fractures. It’s a vicious cycle.
This is where rehabilitation and specific exercises become critically important. Strengthening the back and core muscles, improving balance, and working on posture can make a world of difference in mitigating these effects. It's about retraining your body to support itself as best as it can, even with the structural changes. Your body is amazing at adapting, but it needs a little help sometimes, especially after an injury like this.
The Mobility Maze: Loss of Function and Independence
Let’s be honest, if your back hurts all the time, and you’re not as steady on your feet, your ability to do things you used to enjoy is going to take a hit. For many people, especially older adults, a spinal compression fracture can lead to a significant loss of mobility and independence. Things that were once second nature – like bending down to tie your shoes, reaching for something on a high shelf, or even just getting out of a chair – can become challenging, if not impossible.
This isn’t just about inconvenience; it can be downright isolating. If you can’t get out and about easily, your social life suffers. You might become more reliant on others for basic tasks, which can be difficult for your pride and your sense of self-worth. Think about it: if you can’t do your grocery shopping or play with your grandkids as easily, that’s a huge part of your life that’s suddenly altered.
Furthermore, the fear of falling or re-injuring yourself can become a constant companion, leading to a more sedentary lifestyle. And as we all know, being too sedentary can lead to a host of other health problems, including muscle weakness, weight gain, and an increased risk of cardiovascular disease. It’s a tough cycle to break, and it’s why a proactive approach to recovery and ongoing management is so vital. We want to keep people moving and enjoying their lives for as long as possible, right?
The Mental Game: Fear, Anxiety, and Depression
It’s easy to focus on the physical toll of a spinal compression fracture, but we absolutely cannot ignore the psychological impact. Living with chronic pain, limited mobility, and the fear of future injury can take a serious toll on your mental well-being. Many people experience:
- Anxiety: The constant worry about pain, falls, or re-injury can be overwhelming. You might find yourself constantly on edge, hyper-aware of every movement.
- Depression: The loss of independence, the inability to do things you love, and the ongoing physical discomfort can lead to feelings of sadness, hopelessness, and a lack of interest in life.
- Fear of movement: This is a big one. People become so afraid of causing more pain or injury that they limit their movements drastically. This, ironically, can lead to more weakness and stiffness, perpetuating the problem.
It’s a complex interplay between the physical and the mental. The pain can lead to depression, and depression can amplify the perception of pain. It's a feedback loop that can be incredibly difficult to break out of. This is where support systems – family, friends, support groups, and mental health professionals – become incredibly important. Talking about these feelings, finding ways to cope with stress, and actively working on mental well-being are just as crucial as any physical therapy.
Prevention and Management: Taking the Reins
So, we’ve painted a bit of a stark picture, haven’t we? But here’s the good news: while these long-term effects can be serious, they are not always inevitable, and they can often be managed. The key is a proactive and comprehensive approach.

For those at risk (and let’s be honest, many of us are):
- Bone health is paramount: This means ensuring adequate calcium and vitamin D intake, getting regular exercise (weight-bearing exercises are great!), and avoiding smoking and excessive alcohol consumption. If you’re concerned about osteoporosis, talk to your doctor about screening and potential treatments.
- Fall prevention: This is HUGE. Make your home safer by removing tripping hazards, ensuring good lighting, and installing grab bars where needed. Wear supportive footwear.
- Safe lifting techniques: Even if you’re not lifting heavy objects, using proper form when lifting can save your back.
For those who have experienced a fracture:
- Rehabilitation is your best friend: Work closely with your doctor and physical therapist. A tailored exercise program can help restore strength, flexibility, balance, and posture. Don't skimp on this! It's not just about getting better, it's about staying better.
- Pain management: This might involve medication, but also consider complementary therapies like heat/cold therapy, massage, or even mindfulness techniques.
- Regular check-ups: Keep your doctor informed about how you’re doing. They can monitor your progress and make adjustments to your treatment plan.
- Stay active (safely): Don’t let fear keep you sedentary. Find activities you can do that are safe and enjoyable. Gentle walking, swimming, or even specialized exercise classes designed for people with back issues can be beneficial.
My aunt, after her initial scare, actually got quite involved in a senior’s fitness program that focused on balance and strength. She still complains about her back sometimes, but she’s much more mobile, her posture is better, and she’s not nearly as fatigued. She learned her lesson about trampolining, thankfully, but she also learned that recovery and management are ongoing journeys.
It’s a journey, for sure. But with the right information, support, and a commitment to taking care of yourself, you can significantly mitigate the long-term effects of a spinal compression fracture and get back to living a full and active life. And who knows, maybe you’ll even find a new hobby that’s a little less… gravity-defying.
