What's The Difference Between Osteoarthritis And Rheumatoid Arthritis
Ever feel that little niggle in your knees after a particularly enthusiastic yoga session, or maybe a persistent ache in your fingers after a long afternoon of scrolling through your feed? We’ve all been there. Our bodies, bless their cotton socks, are amazing machines, but sometimes they throw us a few curveballs. And when it comes to joint pain, two big players often come to mind: osteoarthritis and rheumatoid arthritis. They sound a bit similar, don’t they? Like two cousins who look alike but have totally different personalities. Let’s dive in and figure out what’s what, without needing a medical degree, of course!
Think of your joints as the super-smooth hinges that keep your body moving. They’re the magic makers between your bones, allowing you to bend, stretch, and generally conquer the world, one step (or dance move) at a time. But when things go awry with these hinges, it can put a serious damper on your daily groove.
Osteoarthritis: The Wear-and-Tear Tale
So, let’s start with osteoarthritis, or OA. If your joints could talk, OA would be the one sighing and saying, "Oh, these old things? Been through a lot, you know." This is the “wear-and-tear” type of arthritis. It’s the most common kind, and it’s basically your joint’s cartilage saying, "I've had enough!"
Cartilage is that smooth, slippery tissue that cushions the ends of your bones. It’s like the protective padding on a new smartphone screen. When you have OA, this cartilage gradually breaks down. It can become rough, frayed, and eventually, it might disappear altogether, leaving bone rubbing against bone. Ouch.
What causes it? Well, it’s a bit of a mixed bag. Age is a big factor – the older you get, the more likely you are to develop OA. It’s like your joints have been running a marathon for decades, and they’re starting to feel the mileage. Genetics can also play a role; if your parents or grandparents had it, you might be more predisposed.
Then there’s overuse. Think of athletes who've pushed their bodies to the limit, or people whose jobs involve a lot of repetitive joint motion. It’s not about being "fit" or "unfit"; it's about the cumulative stress on those joints over time. Even a past injury, like a sports sprain or a fracture, can make a joint more vulnerable to developing OA later on.
Fun Fact: Did you know that even characters in ancient Egyptian hieroglyphs show signs of osteoarthritis? Talk about a long-standing issue!
What does it feel like? Typically, OA pain is felt during or after movement. You know that stiff, achy feeling you get when you first get out of bed, or after sitting for too long? That's classic OA. It often affects weight-bearing joints like your knees, hips, and spine, but it can also show up in your hands and feet. The stiffness is usually worse in the morning but tends to get better with gentle movement.
It’s usually a gradual onset. You won't wake up one morning with crippling OA. It tends to creep up on you, starting with a mild ache that you might dismiss as "just getting older" or "a bit stiff today." Over time, the pain can become more constant, and you might notice swelling, tenderness, and even a grinding or clicking sensation when you move the joint.

Where does it usually show up? The usual suspects are your knees (making those stairs feel like Everest), your hips (turning over in bed can become an Olympic event), your hands (especially the finger joints closest to your nails and at the base of your thumb), your neck, and your lower back. So, if your hands feel a bit like they’re staging a protest after a long day of texting and scrolling, OA could be the culprit.
What can you do about it? The good news is that while OA can’t be cured, it can be managed. Lifestyle changes are your best friend here. Maintaining a healthy weight is huge. Less weight means less pressure on your joints, especially your knees and hips. Think of it as giving your joints a well-deserved break.
Gentle exercise is also key. It might sound counterintuitive to move a painful joint, but low-impact activities like swimming, cycling, or walking can strengthen the muscles around your joints, providing better support and reducing pain. Tai chi and yoga are fantastic for improving flexibility and balance without putting excessive strain on your joints.
Cultural Connection: In many cultures, especially those with a strong emphasis on physical labor, OA is incredibly common. Think of farmers, construction workers, or even skilled artisans who have spent a lifetime honing their craft with their hands.
Other management strategies include physical therapy, which can teach you specific exercises and stretches. Over-the-counter pain relievers like ibuprofen or naproxen can help manage pain and inflammation. In some cases, your doctor might suggest injections or other treatments.
Rheumatoid Arthritis: The Immune System Hijinks
Now, let’s switch gears and talk about rheumatoid arthritis, or RA. If OA is the grumpy old man of arthritis, RA is the rebellious teenager, or perhaps the overzealous bodyguard. This isn't about wear and tear; it's an autoimmune disease.
What does that mean? It means your immune system, which is supposed to protect you from germs and infections, gets a bit confused. Instead of attacking invaders, it starts attacking your own body, specifically the lining of your joints, called the synovium.

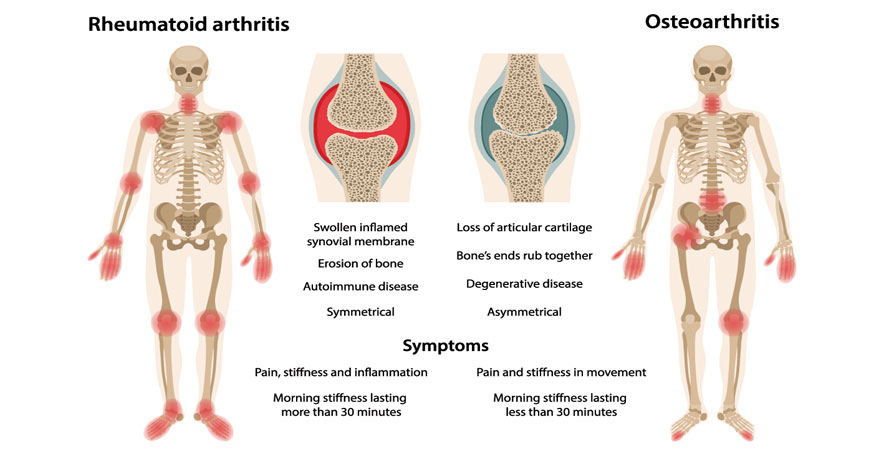
This attack causes inflammation, which can thicken the synovium, leading to joint damage. Over time, this inflammation can erode cartilage and even bone. It can also affect other parts of your body, like your skin, eyes, lungs, and heart.
What causes it? The exact cause of RA is still a bit of a mystery, but it’s believed to be a combination of genetics and environmental factors. Think of it like a perfect storm brewing. You might have certain genes that make you more susceptible, and then an environmental trigger, like a viral infection or even smoking, kicks things off.
Fun Fact: Researchers have found genetic links to RA, suggesting that certain gene variations can increase a person's risk of developing the condition.
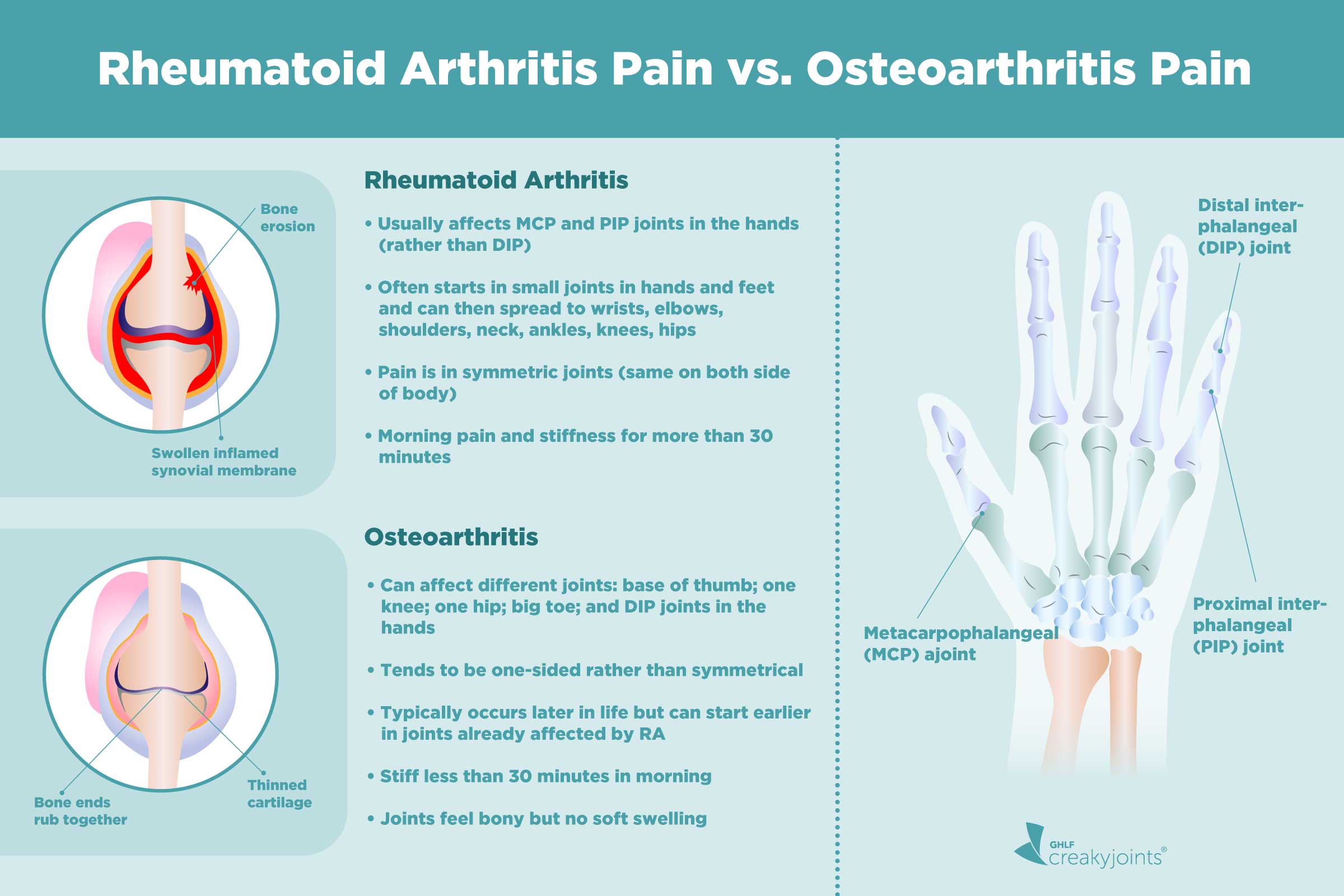
What does it feel like? RA pain often comes with stiffness that is worse in the morning and can last for more than an hour. This morning stiffness is a hallmark of RA. You might feel like your joints are locked up, and it takes a good while for them to loosen up. It's the opposite of OA's morning stiffness that eases with movement. With RA, the initial movement can feel incredibly stiff and painful.
RA often affects joints symmetrically, meaning it tends to appear on both sides of the body. So, if your left wrist is bothering you, chances are your right wrist is feeling it too. It commonly affects smaller joints first, like those in your hands and feet, and then can spread to larger joints.
You might also experience fatigue, which can be profound. It’s not just feeling tired after a long day; it’s a deep, bone-weary exhaustion that can make even simple tasks feel monumental. Other symptoms can include warmth, swelling, and redness in the affected joints, and sometimes even rheumatoid nodules (firm lumps) under the skin.
Where does it usually show up? The most common places for RA to strike are the fingers (especially the middle knuckles and the base of the thumb), the wrists, the elbows, the shoulders, the knees, the ankles, and the toes. It’s less likely to affect your lower back or neck directly in the early stages compared to OA, though it can eventually impact these areas.
What can you do about it? RA is a serious condition that requires medical management. The goal is to control the inflammation, prevent joint damage, and manage symptoms. Treatment often involves a combination of medications, including disease-modifying antirheumatic drugs (DMARDs), which can slow down the progression of the disease, and biologics, which are more targeted treatments.
Lifestyle plays a role too! While medication is crucial, maintaining a healthy lifestyle can significantly improve your quality of life. Gentle exercise, such as swimming or walking, can help maintain joint mobility and muscle strength. A balanced diet is also important for overall health and managing inflammation. Some people find that certain foods seem to trigger flares, so paying attention to your diet might be beneficial.
Cultural Reference: In many Western cultures, particularly with the rise of "wellness" trends, there's a growing awareness of how diet and exercise can impact autoimmune conditions like RA. From turmeric lattes to mindful movement practices, people are exploring holistic approaches alongside medical treatments.
It's also important to listen to your body. If you're experiencing significant fatigue, pacing yourself and getting enough rest is vital. Stress management techniques, like meditation or deep breathing, can also be very helpful, as stress can sometimes exacerbate RA symptoms.
Key Differences at a Glance
Let’s break it down into a super-easy-to-digest format. Imagine your joint is a car.
Osteoarthritis is like the car that’s been driven for a million miles. The parts are worn down from overuse and time. The engine might sputter, the suspension might be a bit rough, and you might hear some creaks and groans when you go over bumps. It’s mainly about the physical breakdown of the "parts" (cartilage).
Rheumatoid Arthritis is like the car where the factory made a mistake, and the car's own security system (immune system) is attacking its own engine parts. The problem isn't just wear and tear; it's an internal malfunction causing damage and inflammation. The car is struggling to run smoothly because its own systems are sabotaging it.
Here’s a quick rundown:
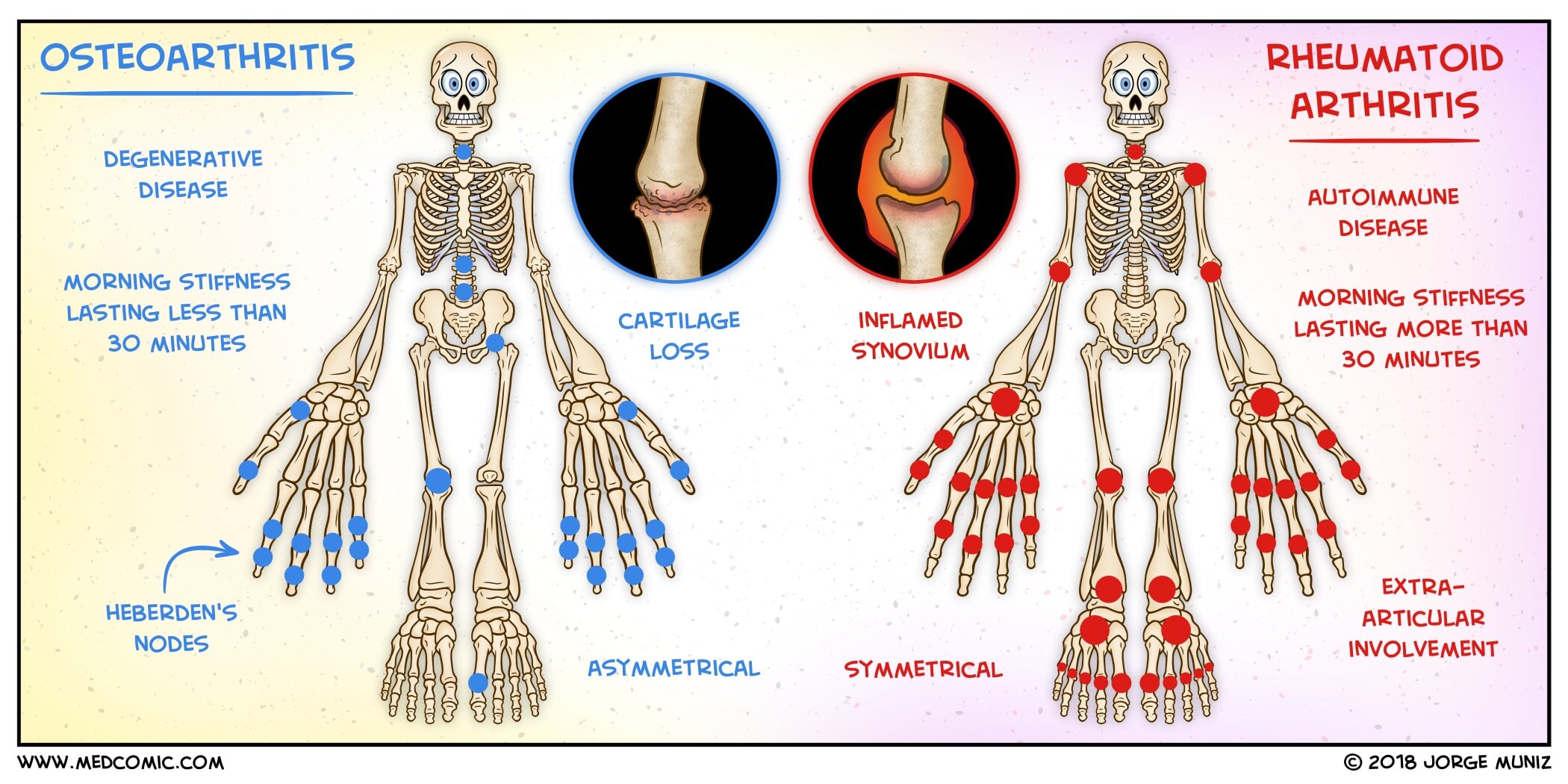
- Cause: OA = Wear and tear; RA = Autoimmune disease (body attacks itself).
- Onset: OA = Gradual; RA = Can be sudden or gradual, often with a general feeling of unwellness.
- Morning Stiffness: OA = Usually less than 30 minutes, improves with movement; RA = Typically longer than an hour, improves with activity.
- Affected Joints: OA = Often one-sided, can affect weight-bearing joints and finger joints; RA = Usually symmetrical, often starts in smaller joints (hands, feet) and can affect multiple joints.
- Systemic Symptoms: OA = Generally localized to joints; RA = Can affect other organs (fatigue, fever, etc.).
A Little Analogy: Think of OA like a favorite pair of jeans that you've worn so much they’ve finally developed holes. RA is more like someone accidentally spilled bleach on your jeans, and now they’re damaged and the color is unevenly affected.
Connecting to Your Daily Life
So, why does all this matter? Because understanding the difference can empower you. If you’re experiencing joint pain, knowing these distinctions can help you have more informed conversations with your doctor and understand the advice you’re given. It’s not just about a diagnosis; it’s about finding the best path forward for your comfort and well-being.
Whether it’s the familiar ache after a long hike (hello, OA!) or the unfamiliar morning stiffness that makes getting out of bed feel like a puzzle (could be RA!), your body is communicating with you. Learning its language, even just the basics of joint health, is a superpower in living an easy-going, active life.
It’s about making conscious choices, like opting for that extra stretch, choosing a brisk walk over the elevator, or simply remembering to stay hydrated. These small, mindful actions are the building blocks of a body that can keep up with your dreams, no matter how many miles it's traveled.
Ultimately, whether your joints are protesting from years of service or staging a small internal protest, the goal is the same: to keep moving, keep enjoying life, and keep those hinges well-oiled, in whatever way works best for you.
